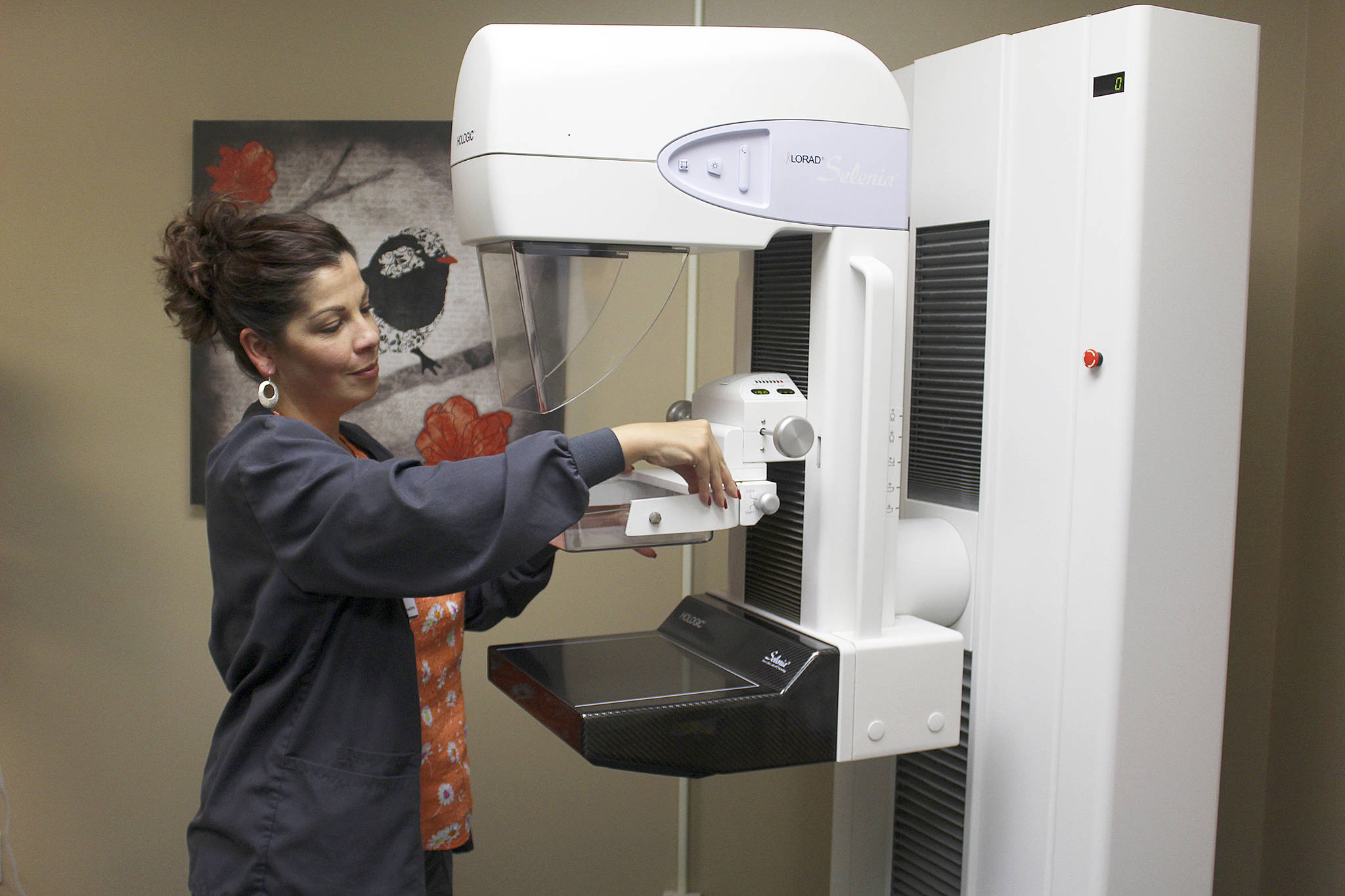
For decades, after receiving mammogram exams, women routinely were handed a reference card on how to perform routine breast self exams as a way to detect lumps or other changes that may be early signs of cancer.
But that’s no longer the recommendation.
“Breast self exam had no effect on long-term mortality,” explained Renee Yanke, oncology manager of WhidbeyHealth Medical Ambulatory Clinic where cancer outpatients receive chemotherapy.
It also led to unnecessary, costly biopsies.
In 2009, the American Cancer Society and U.S. Preventive Service Task Force – two organizations that issue guidelines for breast cancer screening protocols – dropped the blanket recommendation that women conduct a monthly breast self exam, known as BSE.
A meta-analysis study combining the results of the two largest randomized controlled trials comparing women who did routine BSE to those who did not found no difference in breast cancer survival.
Additionally, twice as many biopsies with negative results were done on women who had performed self breast exams, research showed.
“However, that being said, it’s still important to be familiar with your body and with your breasts,” Yanke said. “If you notice something is wrong or different, see a doctor.”
Oftentimes, a woman’s partner is the one who feels or notices changes, she added.
On an average day, between nine to 12 patients come in for mammograms at WhidbeyHealth Medical Center.
The pain of having body parts squashed into unnatural positions between cold, metal plates and told “Don’t breathe. Hold that position,” is an annual rite of pain and passage for women.
However, most women realize the motto “mammograms save lives” is true. About 85 percent of women diagnosed with breast cancer have no prior family history, according to the American Cancer Society.
One tip to lessen discomfort is to take ibuprofen or Advil before going in for a mammogram.
Other standard practices have also been revised in recent years as more as more long-term breast cancer study results are analyzed.
According to American Cancer Society guidelines, age 40 is when a woman of average breast cancer risk should consider beginning annual mammograms. From age 45 to 54, a yearly mammogram is recommended; at age 55, women can opt to have a mammogram every other year.
“Surgery has also changed,” said Dr. Ali Alberton, WhidbeyHealth general surgeon. “We’re doing a lot less surgery and are more selective with performing biopsies.”
Selectively removing one or two lymph nodes instead of a broader sweep results in less complications, experts say.
“More women are opting for breast conservation and we’re able to offer it to more women,” Alberton said.
Women seeking breast reconstruction must travel off Whidbey Island. Most are usually referred to plastic surgeons in Everett.
Outpatient chemotherapy for all types of cancer is provided at WhidbeyHealth’s Medical Ambulatory Clinic, located in a large sunny u-shaped room with sweeping views of its garden. Three Everett Clinic oncologists visit the clinic to provide care. Patients needing radiation therapy, however, must travel to Bellingham, Everett, Seattle or other regional locations.
The incidence of annual Island County new breast cancer cases — 161 cases per 100,000 people — is slightly above the state rate, Alberton said.
How long to continue mammograms as a woman ages into her 80s and 90s is based on several factors, said Dr. Robert Hawkins, the hospital’s medical director of imaging who reviews mammography results.
“A person’s risk of breast cancer keeps going up from age 40 to 90,” he said. Officially, there’s no end age for an elderly woman to forego mammograms, but it’s usually only done if a women is in good health and expected to live another five to 10 years.
Mammogram guidelines
These guidelines are for women at average risk for breast cancer. A woman at average risk doesn’t have a personal history of breast cancer, a strong family history of breast cancer, or a genetic mutation known to increase risk of breast cancer and has not had chest radiation therapy before the age of 30.
Women between 40 and 44 have the option to start mammograms every year.
Women 45 to 54 should get mammograms every year.
Women 55 and older can switch to a mammogram every other year, or they can choose to continue yearly mammograms. Screening should continue as long as a woman is in good health and is expected to live 10 more years or longer.
All women should understand what to expect when getting a mammogram for breast cancer screening – what the test can and cannot do.
Source: American Cancer Society